Cutibacterium acnes (formerly known as Propionibacterium acnes) is the most abundant bacterium in the human skin microbiome, particularly in sebum-rich areas such as the face, scalp, chest, and back. This gram-positive, anaerobic rod-shaped bacterium plays a complex role in skin health, with acne severity now understood to be driven by phylotype-specific metabolic outputs rather than total bacterial load[1]. A landmark 2024 Nature study demonstrated that skin functions as an autonomous lymphoid organ producing local antibodies specifically to constrain C. acnes biomass, with >90% of FOXP3+ Treg cells converting to TFH cells and 90% unique skin BCR clonotypes[2].
Key Characteristics and Phylotypes
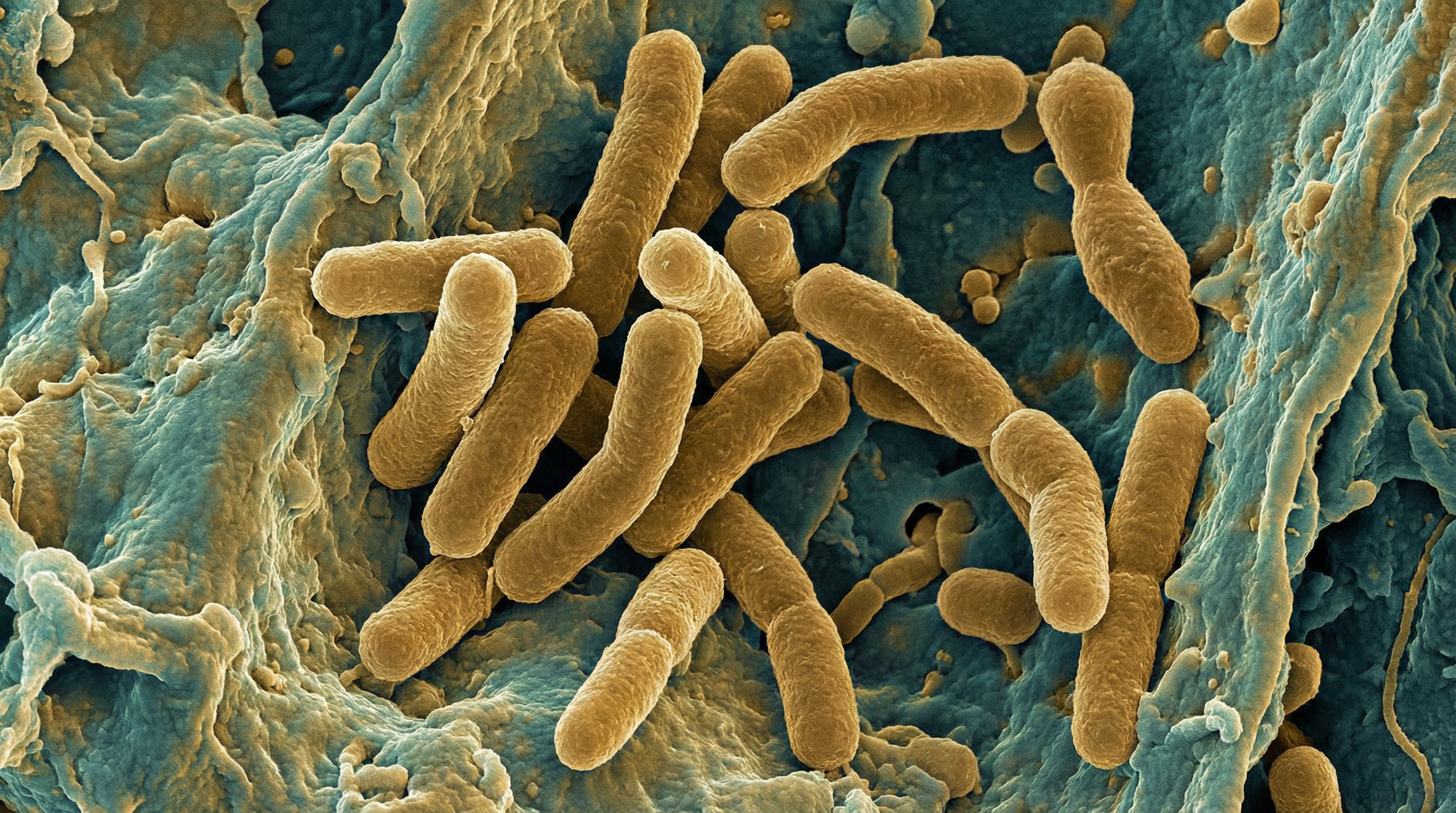
C. acnes is highly adapted to the lipid-rich environment of human skin. The bacterium is classified into phylotypes with dramatically different virulence profiles:
| Phylotype | Association | Key Characteristics |
|---|---|---|
| IA1 | Strongly acne-associated | High virulence; 3.5x higher IL-8; 4x higher porphyrins; DsA1 adhesin; well-structured 3D biofilms |
| IA2 | Deep-seated infections | Forms well-structured biofilms |
| IB | Health-associated | Produces cutimycin antibiotic; anti-inflammatory EVs; only 2 virulence factors in EVs |
| IC | Deep-seated infections | Well-structured 3D biofilms |
| II (C. acnes subsp. defendens) | Health-associated | Higher invasion frequency (72% vs 48%); minimal virulence factors; induces 2.8x higher HBD-2/HBD-3 antimicrobial peptides |
| III | Generally non-pathological | Less defined biofilm structures; rare in infections |
2025 research demonstrated that Phylotype IA1 induces 3.5-fold higher IL-8 secretion and significantly elevated IL-6 and TNF-alpha compared to Phylotype II through aggressive TLR2/MAPK pathway activation[1]. Conversely, Phylotype II induces 2.8-fold higher human beta-defensin 2 (HBD-2) and HBD-3 expression, promoting skin homeostasis through innate immune defenses without excessive inflammation.
Extracellular Vesicles: New Understanding of Pathogenesis
C. acnes-derived extracellular vesicles (EVs) serve as nano-carriers for interkingdom communication with striking phylotype-specific differences[3]:
- IA1 EVs: 3.92 × 10¹² EVs/mL; 96.8 nm diameter; 396 exclusive proteins and 25 virulence factors; consistently upregulate IL-8, IL-6, TNF-alpha, and GM-CSF
- IB/H1 EVs: 100.7 nm diameter; only 2 virulence factors; induce anti-inflammatory IL-10; achieve 4.3-fold reduction in lipid production through acyl-CoA dehydrogenase
These findings suggest EVs from health-associated phylotypes represent potential biotherapy for acne by reducing inflammation without antibiotic side effects.
Porphyrin-ROS-Inflammasome Axis
IA1 isolates produce 4-fold higher coproporphyrin III levels compared to Type II through increased expression of hemE and hemH genes[4]. Porphyrins trigger reactive oxygen species (ROS) production, amplifying inflammatory cascades via:
- Enhanced TLR2/NLRP3 inflammasome activation
- Caspase-1 activation and IL-1β/IL-18 maturation
- Porphyrin production levels now identified as clinical biomarker for acne progression
Biofilm Formation and Prosthetic Joint Infections
Dual-strain communities (IB + II) show nearly double biofilm coverage compared to single strains (27.7% vs 14.3% on titanium discs), with no antagonism observed between phylotypes[5]. Biofilm transcriptomics revealed:
- General reduction in metabolic activity indicating dormancy/quiescence
- Cytochrome bd complex upregulated 5.7-fold—identified as potential therapeutic drug target
- Nitric-oxide reductase (NOR) providing NO protection
- Lysophospholipase (3.6-fold) and hyaluronate lyase (2.6-fold) for tissue invasion
C. acnes causes >10% of all prosthetic joint infections (PJIs) and >50% of shoulder PJIs[6]. The bacterium survives up to 6 months in bone with implant present (only 28 days without), forming biofilms and invading host cells. Contrary to previous belief, C. acnes does NOT evade the immune system at bone sites—but osteoblasts temper the immune response, promoting bacterial persistence.
Skin Autonomous Immunity
A paradigm-shifting 2024 Nature study demonstrated that skin acts as an autonomous lymphoid organ producing local antibodies to constrain C. acnes[2]:
- Langerhans cells capture microbial antigens from hair follicles
- >90% of FOXP3+ Treg cells convert to TFH cells at 21 days post-association
- 80% of skin B cells acquire GCB phenotype by day 14
- 90% unique skin BCR clonotypes with 80% somatic hypermutations
- Formation of dermal tertiary lymphoid organs (TLOs)
- Isotype compartmentalization: lymph nodes (IgG1/IgG3) vs skin (IgG2b/IgG2c)
This means defects in skin-resident B cell responses may increase infection susceptibility even with intact systemic immunity.
Novel Therapeutics
FDA-Approved Innovations
- Clascoterone 1% cream (Winlevi): First topical androgen receptor inhibitor (FDA approved August 2020); competes with DHT for AR binding; 18.4-20.3% success at week 12 vs 6.5-9.0% placebo; first new mechanism since 1982
- Trifarotene 0.005% cream: Fourth-generation retinoid, selective RAR-gamma agonist (FDA approved 2019); effective for facial and truncal acne
- Cabtreo: First FDA-approved triple-combination (clindamycin 1.2%/adapalene 0.15%/BPO 3.1%, 2023)
- Sarecycline: Narrow-spectrum tetracycline targeting C. acnes with reduced gut microbiome disruption (FDA approved 2018)
Bacteriophage Therapy
A Phase 1 clinical trial demonstrated safety of a three-phage cocktail topical application for mild to moderate acne[7]:
- 92-93% metabolic activity restoration with purified phages
- Significant bacterial lysis within 6 hours
- Cell doubling time comparable to non-colonized controls (15.6-15.7h)
- Species-specific targeting with minimal impact on beneficial microbiota
Natural Compounds
Greek Propolis Extract achieved 89.07% biofilm inhibition at 0.5% v/v (comparable to tetracycline's 92.12%)[8]:
- Downregulates virulence genes: CAMP1, CAMP4, roxP, hyl
- Upregulates host antimicrobial factors: IL-4 (55-fold), DEF1B (6-fold)
- Concentrations of 0.1-0.3% preserve skin microbiome biodiversity while targeting C. acnes
Microbiome-Based Approaches
- Live C. acnes subspecies defendens strain XYCM42: Safety evaluation completed; daily application does not cause or exacerbate acne
- Commensal-derived EVs (SLST H1 from Phylotype IB): 4.3-fold reduction in lipid production; anti-inflammatory IL-10 induction
- AviClear 1726-nm laser: FDA approved; selective photothermolysis of sebaceous glands
Therapeutic Paradigm Shift
Understanding phylotype-specific effects has transformed acne treatment strategy:
- Loss of phylotype diversity (IA1 dominance) contributes to inflammatory lesions, not simple bacterial overgrowth
- Maintaining or restoring Phylotype II populations may protect skin barrier by stimulating AMPs without inflammatory cascade
- Personalized "dermatype" therapeutic strategies based on phylotype composition represent the future standard
- Microbiome-preserving therapies should be prioritized over broad-spectrum antibiotics
- Cytochrome bd complex inhibitors represent promising phylotype-agnostic biofilm targets