Optimized Glucose Regulation: Blood Sugar Supplements & Microbiome Strategies
Achieve stable blood sugar levels through microbiome-supported glucose metabolism. Explore glucose lowering supplements, A1C reduction strategies, and evidence-based blood sugar control.
Key Supporting Microbes
These beneficial microorganisms play key roles in supporting this health benefit:
Beyond One-Size-Fits-All Nutrition
One of the most surprising discoveries in nutrition science is that the same food can cause dramatically different blood sugar responses in different people. A banana might spike one person's glucose while barely affecting another's. The key difference? Their gut microbiome[1]. This finding has been validated in multiple populations, demonstrating that personalized nutrition based on microbiome features can effectively predict and improve glycemic responses[5].
This revelation has transformed our understanding of glucose regulation from simple calorie counting to a complex interaction between food, microbiome, and individual physiology.
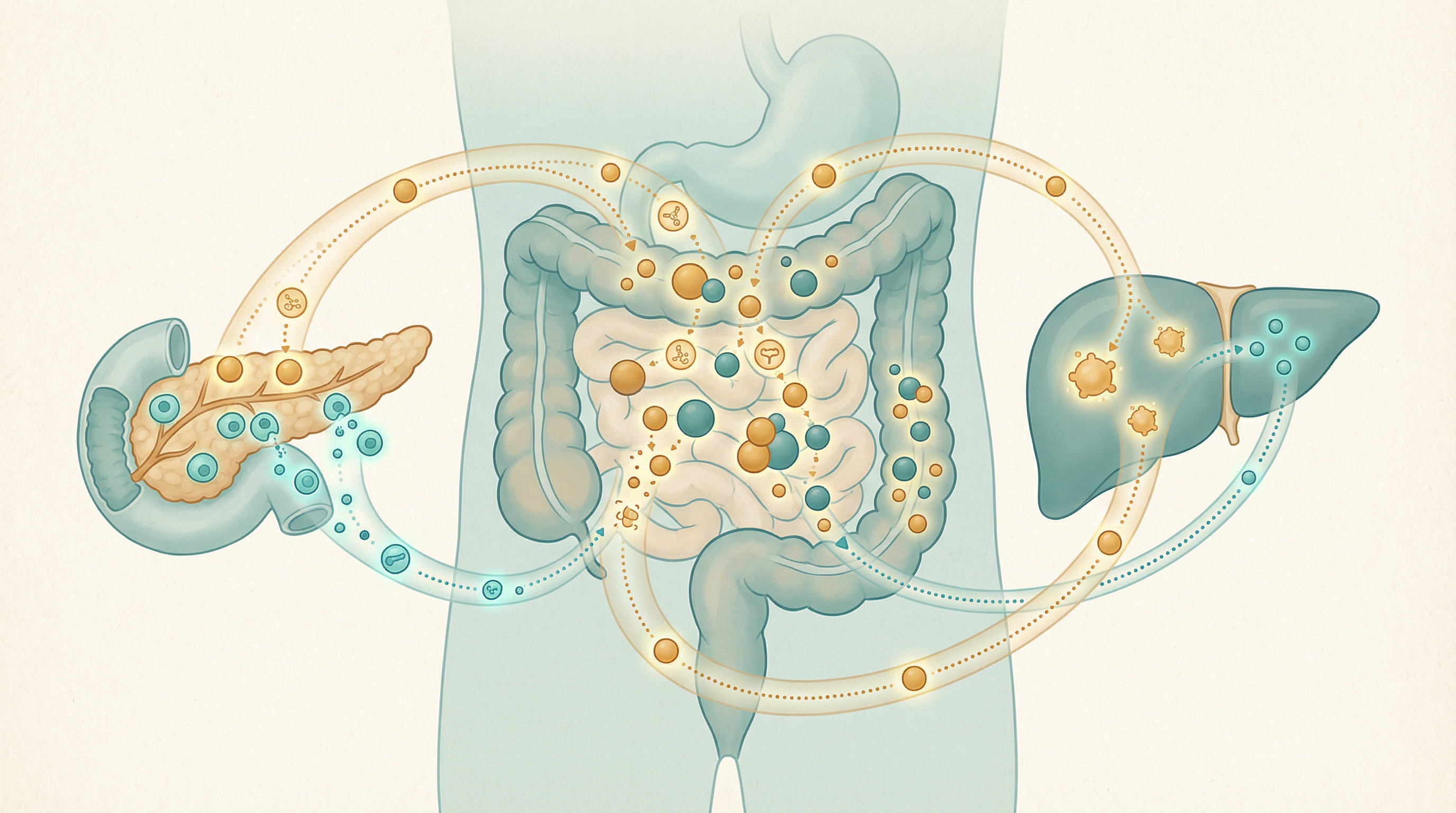
How the Microbiome Regulates Blood Sugar
Incretin Hormone Production
Gut bacteria influence hormones that control glucose[3]:
GLP-1 (Glucagon-like peptide-1):
- Enhances insulin secretion when glucose is high
- Slows gastric emptying, reducing glucose spikes
- Suppresses appetite
- SCFAs from bacterial fermentation stimulate GLP-1 release
GIP (Glucose-dependent insulinotropic peptide):
- Also enhances insulin secretion
- Affected by microbiome composition
- Works synergistically with GLP-1
Short-Chain Fatty Acid Effects
SCFAs improve glucose handling through multiple mechanisms[4]:
- Stimulate incretin hormone release
- Improve insulin sensitivity in tissues
- Reduce hepatic glucose production
- Provide alternative fuel that spares glucose
Bile Acid Signaling
Bacterial bile acid modifications affect glucose:
- Activate FXR, which regulates glucose metabolism
- Activate TGR5, which stimulates GLP-1 release
- Affect how glucose is handled by the liver
- Influence overall metabolic flexibility
Inflammation and Glucose
Gut-driven inflammation impairs glucose control:
- Inflammatory cytokines cause insulin resistance
- LPS from leaky gut worsens glucose tolerance
- Anti-inflammatory bacteria improve glycemic control
- Barrier integrity is essential for glucose regulation
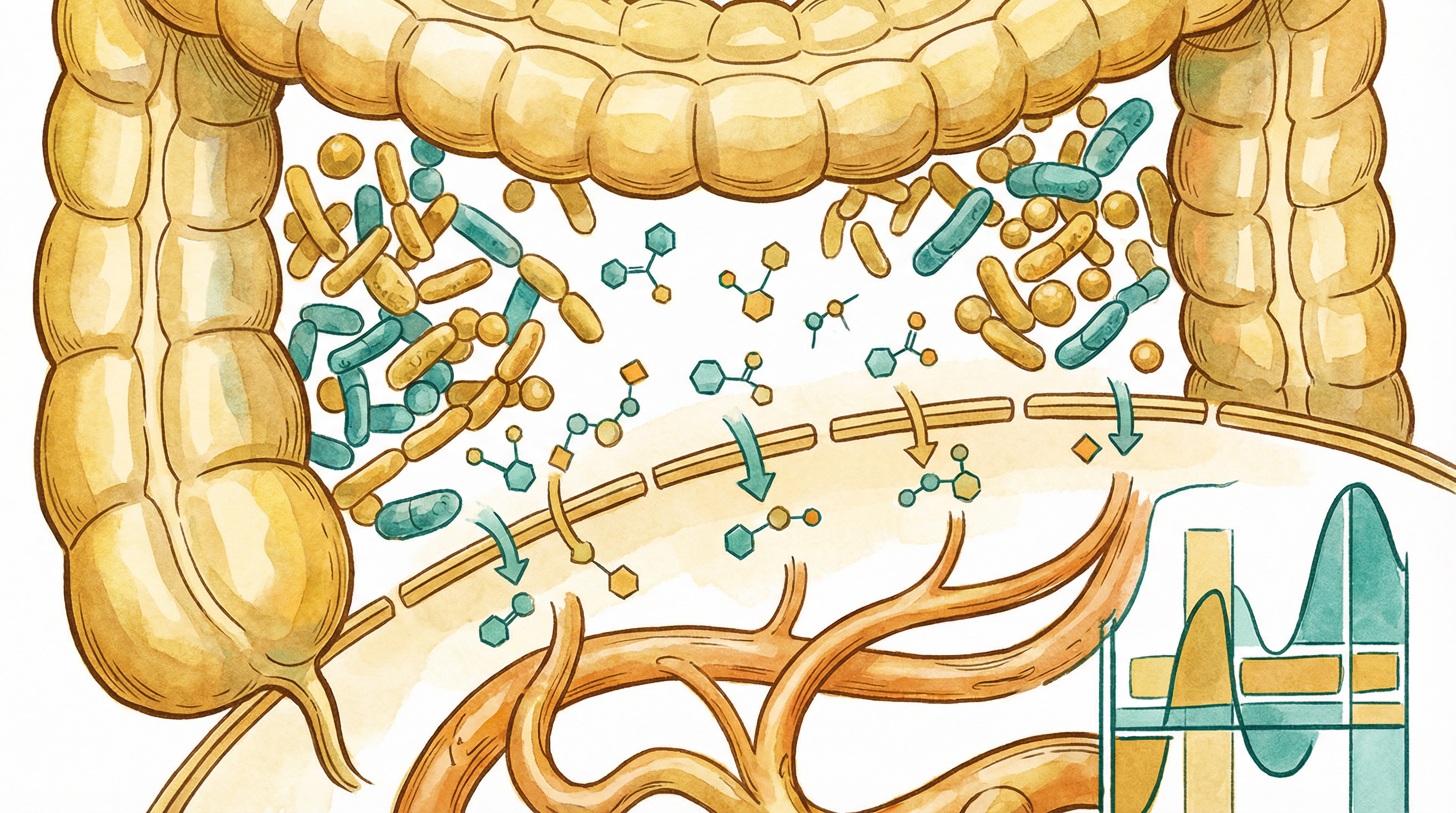
Personalized Glycemic Responses
The Microbiome Connection
Research shows microbiome composition predicts individual glycemic responses[1]:
- People with similar microbiomes respond similarly to foods
- Microbiome features predict glucose spikes better than food composition
- This explains why generic diet advice fails many people
- Personalized approaches based on microbiome show superior results
Factors That Vary Responses
Beyond microbiome, responses depend on:
- Recent meals and overall dietary pattern
- Sleep quality the night before
- Stress levels
- Exercise timing
- Time of day (circadian effects)
- Individual genetics
Key Microbes for Glucose Regulation
Prevotella copri
Complex relationship with glucose[2]:
- Associated with improved glucose tolerance in some contexts
- Particularly beneficial when consuming high-fiber foods
- May worsen glucose in low-fiber, high-fat diets
- Context and diet matter significantly
Bifidobacterium adolescentis
Supports healthy glucose metabolism:
- Produces SCFAs that stimulate incretin release
- Associated with better postprandial glucose control
- Thrives on diverse dietary fiber
- Common in metabolically healthy individuals
Akkermansia muciniphila
Metabolic keystone species:
- Consistently linked to better glucose control
- Improves barrier function, reducing inflammation
- Responds to polyphenols and fiber
- Being developed as a therapeutic probiotic
Eubacterium rectale
Major butyrate producer:
- Supports insulin sensitivity
- Ferments resistant starch effectively
- Often depleted in type 2 diabetes
- Responds well to prebiotic foods
Signs of Poor Glucose Regulation
Watch for these indicators:
- Energy crashes, especially after meals
- Intense sugar cravings
- Difficulty concentrating (brain fog)
- Irritability when hungry ("hangry")
- Excessive thirst or frequent urination
- Slow wound healing
- Frequent infections
- Weight gain, especially abdominal
Dietary Strategies for Glucose Control
Food Order Matters
Simple changes in eating order reduce glucose spikes:
- Vegetables/fiber first — creates a gel that slows absorption
- Protein and fat second — further slows gastric emptying
- Carbohydrates last — absorbed more gradually
This can reduce glucose spikes by 30-40% without changing what you eat.
Fiber with Every Meal
Fiber consistently improves glucose responses:
Soluble fiber:
- Oats and barley
- Legumes
- Apples and citrus
- Psyllium husk
Insoluble fiber:
- Vegetables
- Whole grains
- Nuts and seeds
Resistant starch:
- Cooked and cooled potatoes/rice
- Green bananas
- Legumes
Vinegar and Acidic Foods
Acetic acid blunts glucose responses:
- Apple cider vinegar (1-2 tbsp before meals)
- Fermented foods
- Lemon juice
- Mechanism involves delayed gastric emptying and improved insulin sensitivity
Blood Sugar-Stabilizing Foods
Include regularly:
- Cinnamon (may improve insulin sensitivity)
- Fenugreek
- Bitter melon
- Berberine-containing herbs
- Chromium-rich foods (broccoli, eggs)
Foods to Approach Mindfully
These cause larger glucose responses:
- Refined carbohydrates and white flour products
- Sugary drinks (including fruit juices)
- White rice and potatoes (unless cooled)
- Low-fiber breakfast cereals
- Most processed snack foods

Meal Timing and Glucose
Time-Restricted Eating
Eating within consistent windows improves glucose:
- 8-12 hour eating windows show benefits
- Aligns eating with circadian insulin sensitivity
- Morning meals are typically handled better
- Evening carbohydrates may spike more
Post-Meal Movement
Walking after meals significantly reduces glucose spikes:
- Even 10-15 minutes helps
- Works by increasing glucose uptake into muscles
- Most effective started within 30 minutes of eating
- Light activity is sufficient
Meal Frequency
Evidence is mixed, but consider:
- Fewer, larger meals may be better than constant grazing
- Allows insulin to return to baseline between meals
- May support metabolic flexibility
- Individual responses vary
Lifestyle Factors
Sleep
Poor sleep dramatically worsens glucose control:
- One night of poor sleep reduces insulin sensitivity
- Disrupts hormones that regulate appetite and glucose
- Affects microbiome composition
- Prioritize consistent, quality sleep
Stress
Chronic stress elevates cortisol, which:
- Raises blood glucose directly
- Causes insulin resistance
- Promotes comfort eating of high-sugar foods
- Alters microbiome unfavorably
Exercise
Physical activity improves glucose handling:
- Acute effects: muscles take up glucose during exercise
- Chronic effects: improved insulin sensitivity lasting 24-72 hours
- Both aerobic and resistance training beneficial
- Consistency matters most
Monitoring Your Glucose
Consider these approaches:
- Continuous glucose monitor: Real-time feedback on food responses
- Fasting glucose: Morning measurement
- HbA1c: Average glucose over 3 months
- Oral glucose tolerance test: How you handle a glucose load
- Food-glucose diary: Track patterns in your responses
Building Better Glucose Control
Optimizing glucose regulation through the microbiome involves:
- Prioritizing fiber with every meal
- Strategic food ordering (vegetables → protein → carbs)
- Post-meal movement to enhance glucose uptake
- Time-restricted eating aligned with circadian rhythms
- Supporting beneficial bacteria through prebiotic and fermented foods
- Managing stress and sleep for hormonal balance
Most people notice improved energy and reduced cravings within 2-4 weeks. Measurable improvements in glucose markers typically develop over 2-3 months of consistent practice. Establishing truly optimized glucose metabolism is an ongoing process that improves steadily with sustained effort.
How Much Can A1C Drop in 3 Months?
A1C (HbA1c) reflects average blood glucose over approximately three months, making it a key marker for tracking glycemic improvement. While individual results vary considerably, research suggests that lifestyle interventions combined with microbiome support may contribute to meaningful A1C reductions within a single testing cycle.
What the evidence suggests:
- Dietary changes alone (increased fiber, reduced refined carbohydrates) may help lower A1C by 0.5-1.0% over 3 months in some individuals
- Akkermansia muciniphila supplementation has been associated with improved insulin sensitivity markers in preliminary clinical trials, which may support glycemic improvement over time
- Increased short-chain fatty acid production from prebiotic fiber intake appears to enhance incretin hormone signaling, potentially contributing to better glucose regulation
- Combined approaches (diet, exercise, stress management, microbiome optimization) tend to produce the most consistent results
The microbiome connection to A1C:
- Gut bacteria that produce butyrate and propionate may help improve hepatic insulin sensitivity, which influences fasting glucose and A1C
- Reduced gut permeability (supported by species like Akkermansia) may lower systemic inflammation that contributes to insulin resistance
- Personalized glycemic responses driven by microbiome composition mean that dietary strategies should ideally be tailored to individual biology
It is important to note that A1C management should always involve consultation with a healthcare provider, especially for individuals with type 2 diabetes. Microbiome optimization may complement but should not replace medical treatment.
Blood Sugar Supplements: What Works?
Many people seek supplements to lower blood sugar naturally. While no supplement replaces a healthy diet and lifestyle, some have emerging evidence for supporting glucose metabolism through microbiome-related mechanisms.
| Supplement | Proposed Mechanism | Microbiome Connection | Evidence Level |
|---|---|---|---|
| Berberine | May activate AMPK pathway; appears to support glucose uptake | Appears to increase Akkermansia and Bifidobacterium abundance | Moderate (multiple RCTs) |
| Resistant starch | Feeds SCFA-producing bacteria | Directly enriches butyrate producers like Eubacterium rectale | Strong |
| Inulin/FOS | Prebiotic fiber supporting beneficial bacteria | Increases Bifidobacterium; may enhance GLP-1 secretion | Moderate |
| Chromium | May enhance insulin receptor sensitivity | Limited direct microbiome data | Moderate |
| Cinnamon extract | May improve insulin sensitivity | Some evidence for antimicrobial effects on gut pathogens | Weak to moderate |
| Alpha-lipoic acid | Antioxidant that may support glucose uptake | Limited microbiome research | Moderate |
| Psyllium husk | Soluble fiber that may slow glucose absorption | Supports SCFA production and diverse bacteria | Strong |
Key considerations for glucose lowering supplements:
- Evidence varies significantly by supplement, dose, and individual
- Supplements that support beneficial gut bacteria may offer dual benefits for both microbiome health and blood sugar regulation
- Quality and standardization of supplements vary widely between brands
- Always discuss supplements to lower blood sugar naturally with a healthcare provider, especially if taking diabetes medications, as interactions are possible
Microbiome-first approach to blood sugar supplements: Rather than focusing solely on glucose lowering supplements, consider prioritizing prebiotics and dietary fibers that nourish glucose-regulating bacteria. Resistant starch, inulin, and psyllium husk have the strongest evidence for both microbiome enrichment and glycemic benefit. These blood sugar supplements work by feeding the bacteria that produce metabolites directly involved in glucose regulation.
Supporting Practices
Evidence-based strategies to support this benefit:
- Eat fiber before carbohydrates to blunt glucose spikes
- Take a short walk after meals
- Include vinegar with meals (apple cider vinegar)
- Consume cinnamon regularly
- Practice mindful, slower eating
- Stay well-hydrated throughout the day
Frequently Asked Questions
What is Optimized Glucose Regulation: Blood Sugar Supplements & Microbiome Strategies?
Achieve stable blood sugar levels through microbiome-supported glucose metabolism. Explore glucose lowering supplements, A1C reduction strategies, and evidence-based blood sugar control.
How does the microbiome support optimized glucose regulation: blood sugar supplements & microbiome strategies?
Your gut microbiome plays a crucial role in optimized glucose regulation: blood sugar supplements & microbiome strategies through various mechanisms involving specific beneficial bacteria and their metabolites.
Which microbes are important for optimized glucose regulation: blood sugar supplements & microbiome strategies?
Key beneficial microbes include: Prevotella copri, Bifidobacterium adolescentis, Akkermansia muciniphila, Eubacterium rectale.
References
- Zeevi D, Korem T, Zmora N, et al.. Personalized Nutrition by Prediction of Glycemic Responses. Cell. 2015;163(5):1079-1094. doi:10.1016/j.cell.2015.11.001
- Kovatcheva-Datchary P, Nilsson A, Akrami R, et al.. Dietary Fiber-Induced Improvement in Glucose Metabolism Is Associated with Increased Abundance of Prevotella. Cell Metabolism. 2015;22(6):971-982. doi:10.1016/j.cmet.2015.10.001
- Tolhurst G, Heffron H, Lam YS, et al.. Short-chain fatty acids stimulate glucagon-like peptide-1 secretion via the G-protein-coupled receptor FFAR2. Diabetes. 2012;61(2):364-371. doi:10.2337/db11-1019
- Koh A, De Vadder F, Kovatcheva-Datchary P, Bäckhed F. From dietary fiber to host physiology: Short-chain fatty acids as key bacterial metabolites. Cell. 2016;165(6):1332-1345. doi:10.1016/j.cell.2016.05.041
- Mendes-Soares H, Raveh-Sadka T, Azulay S, et al.. Assessment of a personalized approach to predicting postprandial glycemic responses to food among individuals without diabetes. JAMA Network Open. 2019;2(2):e188102. doi:10.1001/jamanetworkopen.2018.8102