Enhanced Gut-Brain Signaling: Supporting the Gut-Brain Axis
Optimize the bidirectional gut-brain axis communication through microbiome support. Learn practical steps for improving mood, cognition, and stress response via gut-brain signaling.
Key Supporting Microbes
These beneficial microorganisms play key roles in supporting this health benefit:
The Two-Way Conversation
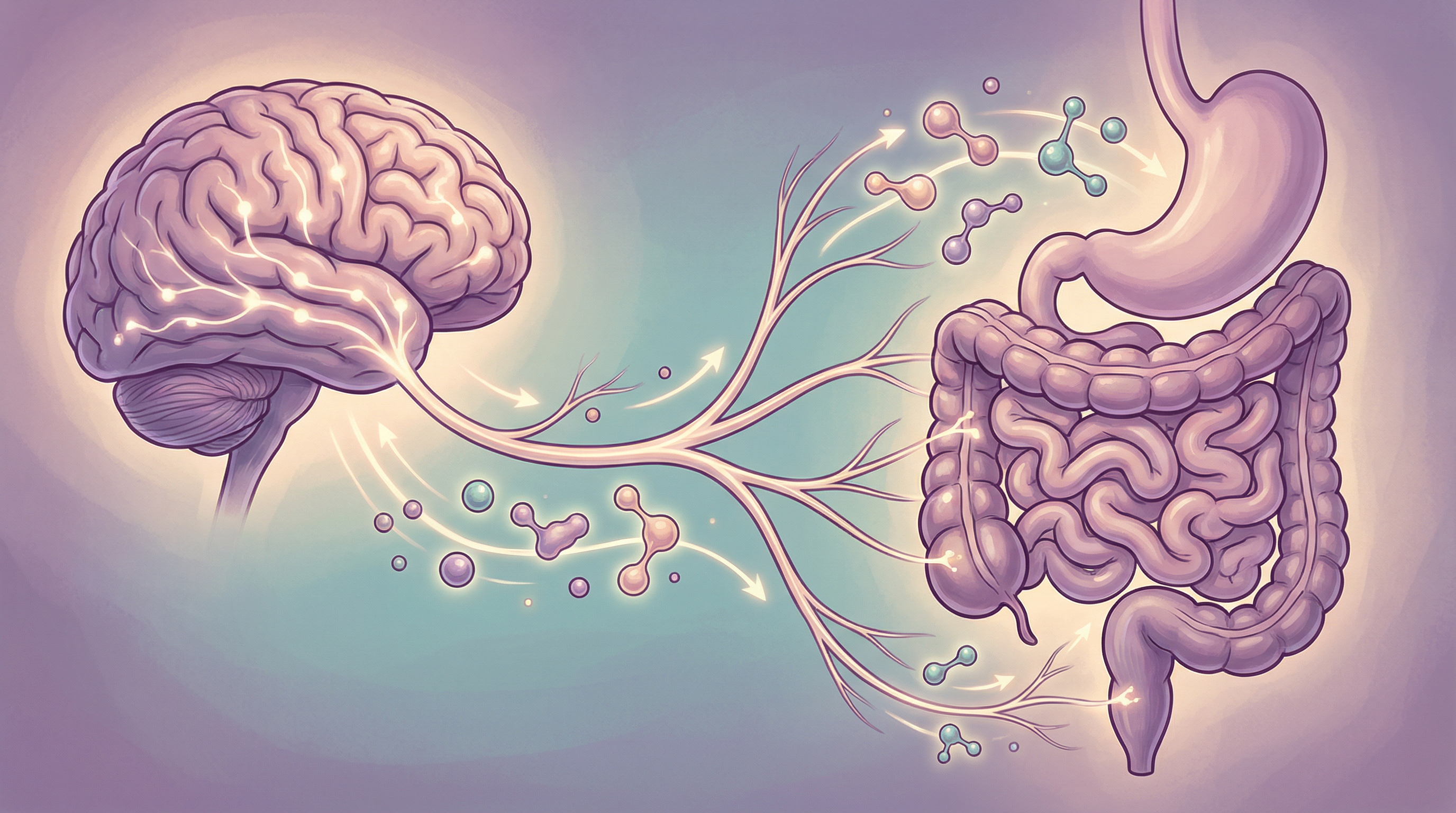
Your gut and brain are in constant communication through a complex network known as the gut-brain axis. This isn't a one-way street—information flows continuously in both directions, with your brain affecting gut function and your gut profoundly influencing your mental state[3].
At the center of this communication network sits your gut microbiome, acting as a critical mediator that can either enhance or disrupt gut-brain signaling. Optimizing this communication is fundamental to mental health and cognitive performance.
The Communication Highways
The Vagus Nerve: The Main Connection
The vagus nerve is the primary neural pathway between gut and brain[2]:
Anatomy:
- Longest cranial nerve in the body
- 80% of its fibers carry signals from gut to brain (afferent)
- 20% carry signals from brain to gut (efferent)
- Directly connects gut bacteria to brain function
Functions:
- Monitors gut environment and conveys status to brain
- Regulates heart rate and breathing
- Controls digestive processes
- Influences mood and stress response
Bacterial influence:
- Certain bacteria activate vagal afferents
- This triggers changes in brain function[1]
- Cutting the vagus nerve blocks many probiotic effects
- Vagal tone correlates with mental health
The Immune Pathway
Immune signaling connects gut inflammation to brain function:
- Cytokines produced in the gut reach the brain
- Immune cells activated in the gut can enter the brain
- Gut inflammation triggers brain immune responses
- Anti-inflammatory bacteria reduce neuroinflammation
The Metabolite Highway
Bacterial metabolites travel via circulation. A comprehensive review in Physiological Reviews characterized this as a complex signaling network involving multiple pathways[4]:
Short-chain fatty acids:
- Cross the blood-brain barrier
- Directly affect brain cells
- Influence neurotransmitter production
- Modulate neuroinflammation
Tryptophan metabolites:
- Affect serotonin availability
- Some are neuroprotective, others neurotoxic
- Balance depends on microbiome composition
Other neuroactive compounds:
- GABA, dopamine precursors
- Histamine
- Various other signaling molecules
The Hormonal System
The hypothalamic-pituitary-adrenal (HPA) axis:
- Regulates stress response
- Is influenced by gut bacteria
- Affects mood and cognition
- Can be dysregulated by dysbiosis
How Bacteria Influence the Brain
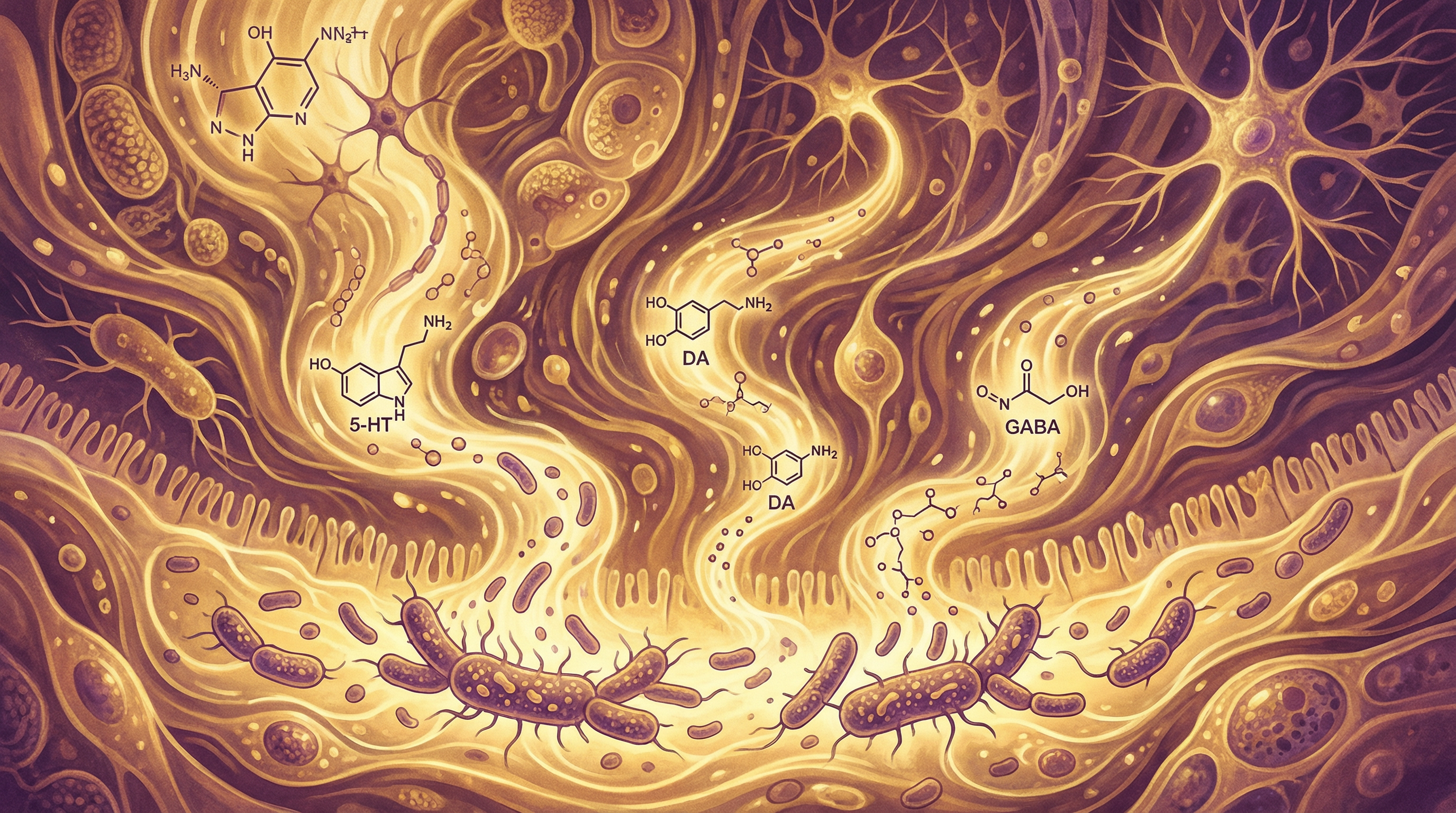
Direct Neurotransmitter Production
Gut bacteria produce neuroactive compounds[5]:
- Serotonin (mostly made in the gut)
- GABA (calming neurotransmitter)
- Dopamine precursors
- Norepinephrine
Vagal Activation
Certain bacteria specifically activate the vagus nerve[1]:
- Lactobacillus rhamnosus changes brain GABA receptors via the vagus
- Bifidobacterium longum reduces stress response through vagal signaling
- These effects disappear if the vagus nerve is cut
Barrier Regulation
Healthy gut-brain signaling requires intact barriers:
- Gut barrier prevents inflammatory leakage
- Blood-brain barrier protects the brain
- Both are influenced by microbiome composition
Immune Modulation
By shaping immune function, bacteria affect brain signaling:
- Anti-inflammatory bacteria reduce brain inflammation
- Pro-inflammatory species increase it
- Balanced immunity supports clear signaling
Signs of Impaired Gut-Brain Communication
You might have disrupted gut-brain signaling if you experience:
- Mood swings unrelated to obvious causes
- Gut symptoms that worsen with stress
- Brain fog or mental clarity issues
- Anxiety or depression with gut involvement
- Stress that triggers digestive upset
- Difficulty with emotional regulation
- Poor stress tolerance
- Fatigue despite adequate sleep
Key Psychobiotic Species
Research on psychobiotics—bacteria that produce mental health benefits—has identified several key species[6]:
Lactobacillus rhamnosus
The most researched psychobiotic:
- Directly activates vagal pathways
- Changes GABA receptor expression in the brain
- Reduces anxiety and depression-like behaviors
- Strain JB-1 particularly well-studied
Bifidobacterium longum
Powerful stress-response modulator:
- Reduces HPA axis activation
- Improves cognitive performance under stress
- Lowers cortisol levels
- Strain 1714 shows anxiolytic effects
Lactobacillus helveticus
Often combined with B. longum:
- Reduces anxiety and depression measures
- Improves sleep quality
- Combination R0052/R0175 is well-researched
- Enhances overall gut-brain communication
Roseburia Species
Important for metabolite signaling:
- Major butyrate producers
- SCFAs directly affect brain function
- Support overall gut-brain axis health
- Respond well to dietary fiber
Strategies to Enhance Gut-Brain Signaling
Vagus Nerve Activation
Deep breathing:
- Slow, diaphragmatic breathing activates the vagus
- Practice 5-10 minutes daily
- Box breathing or 4-7-8 technique
Cold exposure:
- Cold showers or face immersion
- Activates vagal response
- Start gradually
Singing, humming, gargling:
- Activate vagal motor fibers
- Simple and accessible
- Practice regularly
Meditation:
- Increases vagal tone
- Improves gut-brain communication
- Multiple techniques effective
Dietary Support
Fermented foods:
- Introduce psychobiotic species
- Support overall microbiome health
- Include variety (yogurt, kefir, sauerkraut, miso)
Fiber for SCFA production:
- Diverse plant fibers
- Resistant starch
- Prebiotic-rich foods
Omega-3 fatty acids:
- Support neuronal membrane health
- Have anti-inflammatory effects
- May enhance vagal function
Polyphenols:
- Feed beneficial bacteria
- Have direct neuroprotective effects
- Include berries, green tea, dark chocolate
Lifestyle Factors
Exercise:
- Enhances vagal tone
- Improves microbiome diversity
- Reduces stress hormones
- Boosts brain-derived neurotrophic factor
Sleep:
- Essential for gut-brain axis function
- Supports microbiome circadian rhythms
- Allows neural restoration
Stress management:
- Chronic stress impairs gut-brain communication
- Mind-body practices restore balance
- Social connection is protective
Nature exposure:
- Contact with nature reduces stress
- May diversify the microbiome
- Improves overall well-being
Testing Gut-Brain Function
Assessment options include:
- Heart rate variability: Measures vagal tone
- Cortisol testing: Shows HPA axis function
- Microbiome testing: Reveals psychobiotic abundance
- Inflammatory markers: Indicate gut-brain inflammation
- Neurotransmitter metabolites: Show production patterns

Building Better Communication
Enhancing gut-brain signaling through the microbiome involves:
- Supporting psychobiotic species through diet and potentially supplements
- Activating the vagus nerve through breathing, cold exposure, and other practices
- Reducing inflammation that disrupts signaling
- Managing stress which impairs gut-brain communication
- Maintaining healthy barriers to ensure clean signal transmission
Most people notice improvements in mood, stress response, and mental clarity within 4-8 weeks of consistent gut-brain supporting practices. Optimizing this complex communication network is an ongoing process that deepens over months of sustained effort.
How to Support the Gut-Brain Axis
The gut-brain axis is a bidirectional communication network that profoundly influences mental health, cognitive function, and emotional resilience. Supporting this brain axis connection requires a multi-faceted approach that addresses both the gut microbiome and neural signaling pathways.
Step 1: Nourish Your Psychobiotic Bacteria
The gut-brain axis depends on having the right bacteria to produce neuroactive compounds:
- Eat diverse fermented foods daily: Yogurt, kefir, kimchi, and miso introduce and support psychobiotic species that modulate the gut-brain axis
- Prioritize prebiotic fibers: Inulin, FOS, and resistant starch feed SCFA-producing bacteria that support brain axis signaling
- Include omega-3 fatty acids: Found in fatty fish, walnuts, and flaxseed; these may support both neuronal health and beneficial bacteria growth
- Consume polyphenol-rich foods: Berries, green tea, dark chocolate, and red grapes feed bacteria that produce neuroprotective metabolites
Step 2: Strengthen the Vagus Nerve
The vagus nerve is the primary physical connection of the gut-brain axis. Strengthening vagal tone enhances this brain axis communication:
- Practice daily deep breathing: 5-10 minutes of slow diaphragmatic breathing (inhale 4 seconds, hold 7, exhale 8) directly stimulates vagal afferents
- Try cold exposure: Brief cold showers (30-60 seconds at the end of a warm shower) activate the vagal response and may improve stress resilience
- Sing, hum, or gargle: These activities activate vagal motor fibers in the throat, enhancing gut-brain axis tone
- Meditate regularly: Even 10 minutes daily has been shown to increase vagal tone and improve gut-brain axis communication
Step 3: Reduce Gut-Brain Axis Disruptors
Certain factors impair the gut-brain axis and should be minimized:
- Chronic stress: Directly suppresses vagal function and alters microbiome composition; implement daily stress management practices
- Ultra-processed foods: May promote inflammatory gut bacteria that produce neurotoxic metabolites, disrupting brain axis signaling
- Sleep deprivation: Disrupts microbiome circadian rhythms and impairs neural restoration; aim for 7-9 hours nightly
- Excessive alcohol: Increases gut permeability, allowing inflammatory compounds to reach the brain
Step 4: Consider Targeted Psychobiotic Support
For those seeking additional gut-brain axis support:
- Lactobacillus rhamnosus JB-1: Changes GABA receptor expression in the brain via vagal signaling
- Bifidobacterium longum 1714: Reduces cortisol and improves cognitive performance under stress
- L. helveticus R0052 + B. longum R0175: Well-studied combination for anxiety and depression symptom support
For a comprehensive exploration of the science behind the gut-brain axis, see our article on the gut-brain connection. For broader strategies on supporting mental health through the microbiome, explore our mental health goal pathway.
Supporting Practices
Evidence-based strategies to support this benefit:
- Practice deep breathing exercises to stimulate the vagus nerve
- Include fermented foods to support psychobiotic bacteria
- Engage in regular physical activity
- Practice mindfulness meditation
- Cold exposure (cold showers) to enhance vagal tone
- Humming or singing to activate the vagus nerve
Frequently Asked Questions
What is Enhanced Gut-Brain Signaling: Supporting the Gut-Brain Axis?
Optimize the bidirectional gut-brain axis communication through microbiome support. Learn practical steps for improving mood, cognition, and stress response via gut-brain signaling.
How does the microbiome support enhanced gut-brain signaling: supporting the gut-brain axis?
Your gut microbiome plays a crucial role in enhanced gut-brain signaling: supporting the gut-brain axis through various mechanisms involving specific beneficial bacteria and their metabolites.
Which microbes are important for enhanced gut-brain signaling: supporting the gut-brain axis?
Key beneficial microbes include: Lactobacillus rhamnosus, Bifidobacterium longum, Lactobacillus helveticus, Roseburia species.
References
- Bravo JA, Forsythe P, Chew MV, et al.. Ingestion of Lactobacillus strain regulates emotional behavior and central GABA receptor expression in a mouse via the vagus nerve. Proceedings of the National Academy of Sciences. 2011;108(38):16050-16055. doi:10.1073/pnas.1102999108
- Bonaz B, Bazin T, Pellissier S. The Vagus Nerve at the Interface of the Microbiota-Gut-Brain Axis. Frontiers in Neuroscience. 2018;12:49. doi:10.3389/fnins.2018.00049
- Mayer EA, Tillisch K, Gupta A. Gut/brain axis and the microbiota. Journal of Clinical Investigation. 2015;125(3):926-938. doi:10.1172/JCI76304
- Cryan JF, O'Riordan KJ, Cowan CSM, et al.. The Microbiota-Gut-Brain Axis. Physiological Reviews. 2019;99(4):1877-2013. doi:10.1152/physrev.00018.2018
- Dinan TG, Cryan JF. Gut instincts: microbiota as a key regulator of brain development, ageing, and neurodegeneration. The Journal of Physiology. 2017;595(2):489-503. doi:10.1113/JP273106
- Sarkar A, Lehto SM, Harty S, et al.. Psychobiotics and the Manipulation of Bacteria-Gut-Brain Signals. Trends in Neurosciences. 2016;39(11):763-781. doi:10.1016/j.tins.2016.09.002